By Chris Neil, Critical Care Paramedic
Asthma is a disease of predominantly reversible airway obstruction resulting from a triad of bronchoconstriction, bronchial mucosal oedema and mucus plugging. For the majority, control of asthma symptoms is readily achieved; however there are approximately 1,400 asthma deaths in the UK each year. Most of these deaths occur in the pre-hospital setting, and in retrospect the majority are considered preventable.
Tip 1: know how these patients may present to you
A progressive worsening of symptoms over several days; with reports of nocturnal dyspnoea in the previous three nights. As a result of greater bronchial inflammation and mucous secretion, this group (occurring more frequently in females) tends to respond more slowly to treatment.
A smaller sub-group, more frequently male, present with a rapidly progressive condition with reactive airways. These patients have intense bronchospasm that often responds more rapidly to bronchodilator therapy. This group are often referred to as brittle asthmatics.
Tip 2: be familiar with the presenting features of life threatening asthma
They may vary but will include one or more of the following:
Tip 3: think adrenaline
Essentially the only drug with an evidence base for life-threatening asthma is IM adrenaline 1:1000 (0.5mg) and should be considered immediately after recognising this life-threatening condition.
Refer to your JRCALC clinical guidelines 2014 pocket book if unsure about adrenaline dose. So far there are no documented cases of an intra-cerebral haemorrhage from IM adrenaline 1:1000 (0.5mg).
Tip 4: administer adrenergic receptor agonists; salbutamol 2.5-5mg (nebulised with O2).
High doses of adrenergic receptor agonists can cause tachycardia and hypokalaemia and therefore patients should be continually visually and mechanically monitored.
Tip 5: formulate a plan
Don’t delay extrication or transportation with meaningless intervention. Can the patient be safely extricated in a timely fashion? Consider calling the critical care desk on talk group 202 or call 01245 444496 to request critical care.
Specialist paramedics trained in critical care can administer magnesium sulphate and HEMS teams can provide advanced airway management and ventilation for these patients. Magnesium sulphate causes smooth muscle relaxation and is thought to modulate the inflammation.
Tip 6: look at assisted ventilation
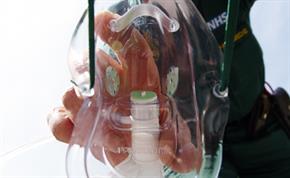
Patients with life-threatening asthma can soon become exhausted and may require assisted ventilation with in-line nebulisation connected to a BVM.
The positive pressure will help to re-recruit collapsed bronchioles and alveoli, and improve gas exchange. Assisted ventilation in this situation requires a different approach and the following should be considered:
1. Be familiar with the in-line nebuliser with BVM and HME filter.
2. Assisted ventilation with BVM is ideally a two person operation. Try to maintain a tight facemask and coordinate ventilation in response to the patient’s breathing pattern.
3. Attempts should be made to keep the patient in a sitting position to maintain functional residual capacity (if the patient is in cardiac arrest position the patient supine during resuscitation attempts).
4. Higher inflation pressures may be required if chest compliance is poor. ‘Air trapping/ air stacking’ may occur and time should be allowed for gas to escape from the chest after each inspiration. This can be achieved by modifying the inspiration expiration ratio (I: E) to 1:4. This can also be achieved by modifying the ventilatory rate to 6-8 breaths per minute with a slow inspiration. If the chest becomes hyperinflated, attempts to ‘decompress’ the chest by manually squeezing the chest on occasion may help.
5. Rate of pneumothorax in life threatening asthma is around 1:100 so this needs to be actively assessed for.
6. Altered level consciousness maybe due to hypoxia and hypercarbia.
Tip 7: look at second line management strategies
Administer hydrocortisone 100 mg IV; hydrocortisone can take up to five hours to have an effect and should not delay extrication or transportation.
Administer ipratropium bromide; 0.5mg (can be mixed with salbutamol and nebulised with O2).
Administer IV fluid; these patients are often dehydrated and therefore have intravascular depletion, coupled with high intrathoracic pressures can result in hypotension. Fluid loading in increments 250ml is often required.
Tip 8: provide the receiving hospital with an early ATMISTER report
Example:
Age: 22-year-old male
Time: acute onset at 10:00 hrs
Mechanism: respiratory distress
Injury: impression is life threatening asthma
Signs: silent chest, resps 38, sats 91% on oxygen, BP 98/60, pulse 133 & GCS 13, E3 V4 M6
Treatment: IM adrenaline, oxygen, salbutamol and IV fluids
ETA: 10 minutes
Requests: anaesthetics please
For more information see your JRCALC pocket book or your Clinical Manual 2014.